Stem cells show power to predict disease, drug toxicity
For the first time, scientists have used human embryonic stem cells to predict the toxic effects of drugs and provide chemical clues to diagnosing disease.
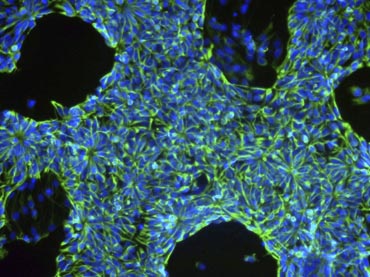
Microscopic view of neural precursor cells from the research lab of Gabriela Cezar,UW-Madison professor of animal science. The cells were derived from human embryonic stem cells and were exposed to a drug known to cause autism in a small percentage of cases. By assessing the small-molecule chemicals expressed by the cells when they are exposed to the drug, scientists can gain fundamental insight into the toxic effects of drugs on cells in development.
Photo: courtesy Gabriela Cezar
Writing this week in the journal Stem Cells and Development, a team led by UW–Madison biologist Gabriela Cezar reports the use of all-purpose stem cells to elicit and identify the telltale chemical signals secreted by the cells when exposed to a drug known to cause autism.
The work is important because it is a critical first step toward fulfilling the promise of embryonic stem cells not only to screen drugs for safety but one day, possibly, to use the cells themselves as crucibles for making new drugs. What’s more, the work shows that stem cells have an immediate clinical application as they generate chemicals, biomarkers, that can be used to predict the onset of disease, much like cholesterol or sugar in the blood can be used to forecast heart disease or diabetes.
"We’re measuring active metabolites produced by the cells in response to an insult," explains Cezar, a UW–Madison professor of animal science. "These are de facto signatures of what is happening in response to a drug or a disease state."
In the new study, Cezar and her colleagues measured the response of undifferentiated stem cells as well as precursor neural cells to the drug valproate, which is known to cause autism in the offspring of a small percentage of users. The drug is used to treat epilepsy, bipolar disease and migraine headaches.
Cells exposed to the drug, according to the new study, secreted more of the small-molecule chemicals involved in development and in brain cell signaling than unexposed cells.
"Some of the chemicals we detected are critical for formation of the brain," Cezar explains. "It seems the drug may induce excess chemicals that alter neural development."
An increase in glutamate metabolism in cells exposed to valproate, for example, may be a critical clue to understanding what goes wrong in development to cause autism: "Excess glutamate kills neurons," says Cezar. "If you have higher levels during the formation of the brain, you may have fewer neurons of different types. In autism, there are areas of the brain where you have fewer neurons" than would occur under ordinary circumstances.
"Autism is a condition that begins during pregnancy," notes Cezar. "In this study, we asked what could valproate tell us about autism given its known involvement in a small percentage of cases? How does it make brain development different?"
Cells of all kinds use so-called small-molecule chemicals as a way to communicate with other cells. Precise communication between cells is essential for normal development and the health of an organism. Such chemicals can be detected in blood, suggesting it may be possible to devise simple tests that can provide disease diagnosis before birth or shortly after.
"These are small molecules that are indicators of susceptibility to disease," says Cezar.
The work by Cezar and her colleagues, including noted central nervous system expert Fred Gage of the Salk Institute, opens a raft of possibilities for early disease diagnosis of developmental disorders. In short, the ability to tune in to the chemical chatter of stem cells may become a promising new window to helping scientists figure out, at the most fundamental level, what goes wrong to cause things such as birth defects and miscarriage.
In addition, the work shows how human embryonic stem cells and early precursor cells can be used to screen drugs for potentially harmful effects. Drug discovery and testing had been predicted to be one of the first technologies to emerge from embryonic stem cells.
In terms of drug discovery and screening, human cells offer an alternative to animal testing that may be more accurate and could help ferret out safety issues that animal models fail to identify.
The new study was supported in part by grants from the Draper Technology Innovation Fund and the UW–Madison Graduate School.
In addition to Cezar and Gage, authors of the new study include Jessica A. Quam, Alan M. Smith, Guilherme J.M. Rosa, and James F. Brown, all of UW–Madison; Marian S. Piekarczyk of the WiCell Research Institute; and Alysson R. Muotri of the Salk Institute.
Tags: business, research, stem cells




