Wisconsin team grows retina cells from skin-derived stem cells
A team of scientists from the School of Medicine and Public Health has successfully grown multiple types of retina cells from two types of stem cells — suggesting a future in which damaged retinas could be repaired by cells grown from the patient’s own skin.
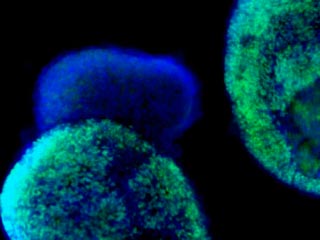
A team of scientists led by David Gamm, assistant professor of ophthalmology and visual sciences, and Jason Meyer, research scientist, has successfully grown multiple types of retina cells from two types of stem cells — suggesting a future in which damaged retinas could be repaired by cells grown from the patient’s own skin. Pictured here in a microscopic photograph are early retinal cells (green) and early brain cells (blue).
Even sooner, the discovery will lead to laboratory models for studying genetically linked eye conditions, screening new drugs to treat those conditions and understanding the development of the human eye.
A Waisman Center research team led by David Gamm, an assistant professor of ophthalmology and visual sciences, and Jason Meyer, a research scientist, announced its discovery in the Aug. 24 edition of the Proceedings of the National Academy of Sciences.
“This is an important step forward for us, as it not only confirms that multiple retinal cells can be derived from human iPS cells using the Wisconsin approach, but also shows how similar the process is to normal human retinal development,” Gamm says. “That is quite remarkable given that the starting cell is so different from a retinal cell and the whole process takes place in a plastic dish. We continue to be amazed at how deep we can probe into these early events and find that they mimic those found in developing retinas. Perhaps this is the way to close the gap between what we know about building a retina in mice, frogs and flies with that of humans.”
Gamm says the work built on the strong tradition of stem cell research at UW–Madison. James Thomson, a School of Medicine and Public Health faculty member and director of regenerative medicine at the Morgridge Institute for Research on the UW–Madison campus, announced that he had made human stem cells from skin, called induced pluripotent stem (iPS cells), in November 2007.
Su-Chun Zhang, UW–Madison professor of anatomy and a Waisman researcher, was among the first to create neural cells from embryonic stem cells. Zhang was also part of the Gamm lab’s retinal study. Meyer says the retina project began by using embryonic stem cells, but incorporated the iPS cells as they became available.
Ultimately, the group was able to grow multiple types of retina cells beginning with either type of stem cell, starting with a highly enriched population of very primitive cells with the potential to become retina. This is critical, as it reduces contamination from unwanted cells early in the process.
In normal human development, embryonic stem cells begin to differentiate into more specialized cell types about five days after fertilization. The retina develops from a group of cells that arise during the earliest stages of the developing nervous system. The Wisconsin team took cells from skin, turned them back into cells resembling embryonic stem cells, then triggered the development of retinal cell types.
“This is one of the most comprehensive demonstrations of a cell-based system for studying all of the key events that lead to the generation of specialized neural cells,” Meyer says. “It could serve as a foundation for unlocking the mechanisms that produce human retinal cells.”
Because the group was successful using the iPS cells, they expect this advance to lead to studying retinal development in detail and treating conditions that are genetically linked. For example, skin from a patient with retinitis pigmentosa could be reprogrammed into iPS cells, then retina cells, which would allow researchers to screen large numbers of potential drugs for treating or curing the condition.
Likewise, someday ophthalmologists may be able to repair damage to the retina by growing rescue or repair cells from the patient’s skin. Earlier this year, scientists from the University of Washington showed that human ES cells had the potential to replace retinal cells lost during disease in mice.
“We’re able to produce significant numbers of photoreceptor cells and other retinal cell types using our system, which are lost in many disorders,” Meyer says. Photoreceptors are light-sensitive cells that absorb light and transmit the image as an electrical signal to the brain.
The team had similar success in creating the multiple specialized types of retina cells from embryonic stem cells, underscoring the similarities between ES and iPS cells. However, Gamm emphasizes that there are differences between these cell types as well. More work is needed to understand their potential and their limitations.
Other members of Gamm’s Waisman Center research team involved in this study include Elizabeth Capowski, Lynda Wright, Kyle Wallace, Rebecca Shearer and Erin McMillan.
The research was funded by the National Institutes of Health, the Foundation Fighting Blindness, the Walsh Family Foundation, the Lincy Foundation and the Retina Research Foundation.




