Wireless microcamera clusters broaden laparoscopic imaging
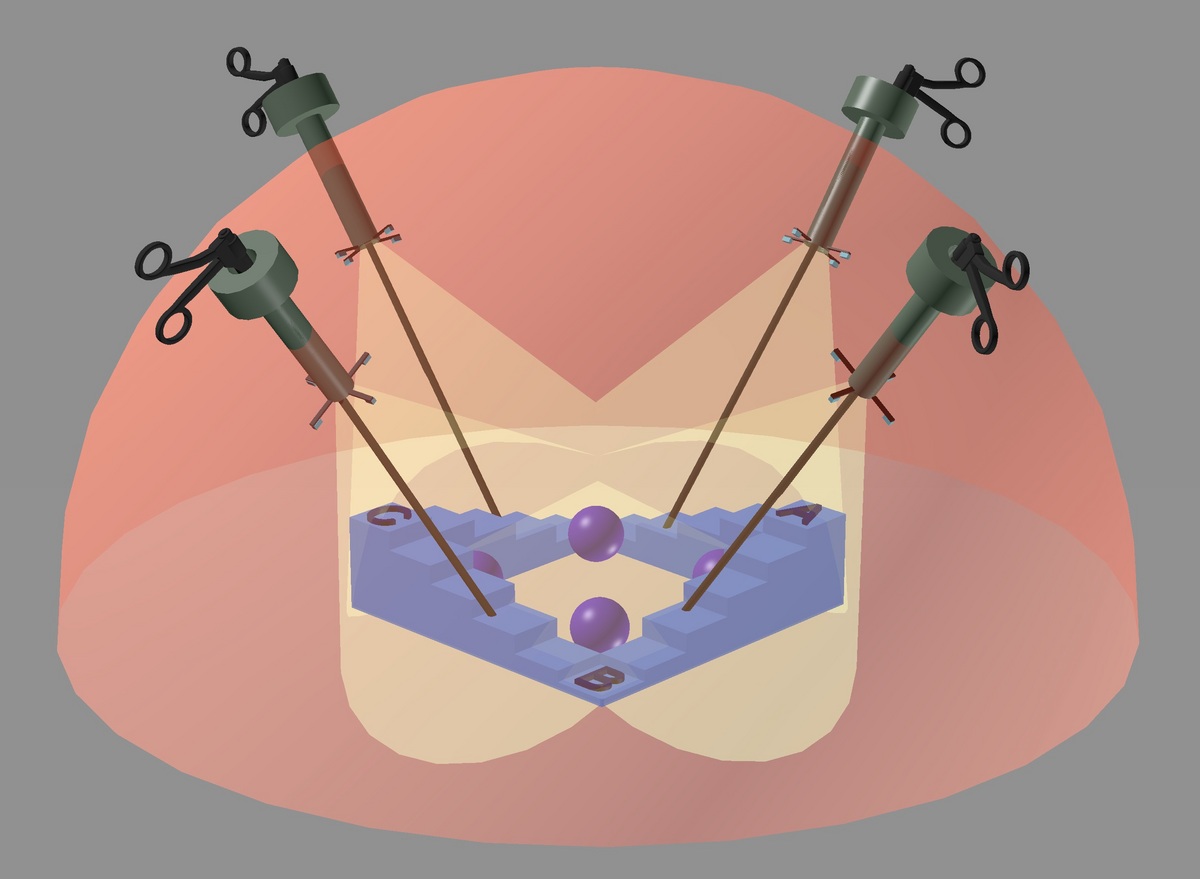
The innovative laparoscopic imaging system features retractable camera arrays affixed to the lower end of each port inserted into a patient’s abdomen. The system provides surgeons a 3-D view of the site of the procedure and allows them to insert surgical instruments through any of the ports. In this image, the balls and letters A, B and C represent objects at different locations and focal planes in the surgical field.
Image courtesy of Hongrui Jiang group
A revolutionary integrated imaging system under development at the University of Wisconsin–Madison could significantly advance laparoscopy, a minimally invasive surgical procedure that, over the last half century, has seen only incremental improvements in imaging.
The system takes advantage of variable focal length microlens systems pioneered by Hongrui Jiang, the Lynn H. Matthias and Vilas Distinguished Achievement Professor of electrical and computer engineering at UW–Madison.

Hongrui Jiang
Laparoscopy is a minimally invasive technique used for procedures in the abdominal area, including surgery on the colon, stomach, esophagus or reproductive organs, among many others. A surgeon conducts the procedure with the assistance of a video camera and long, thin instruments fed through three to five ports, or trocars, placed in small incisions in the abdomen.
In most current laparoscopic procedures, the camera presents several challenges — one of which is that the surgeon can’t operate it independently, says Charles Heise, a UW–Madison professor of surgery. “Another person must hold the camera, manipulate it, focus it, and move it in and out to clean it,” he says. “It has a limited field of view and it ties up one of the ports.”
The new system centers around retractable microlens arrays — essentially, miniature wireless video cameras — integrated onto the end of each port. When a port is inserted into the body, these cameras will flare out in a ring, allowing the surgeon to use the port simultaneously for imaging and operating. Using software or voice commands, the surgeon can tune the focus of each camera to adjust the depth of field, which improves the image quality. Multiple cameras on each port will provide an immersive, three-dimensional view of the procedure, yet their location near the abdominal wall will help to minimize spatter that ordinarily would accumulate on a traditional camera placed right at the site of the procedure.

Charles Heise
Jiang says the new system is a holistic solution that addresses most of the drawbacks in the current technology. “Rather than address incremental improvements, we came up with a paradigm shift to address all of the problems surgeons experience,” he says. “We’re taking advantage of the ports that already are there. Our cameras are deployed with and close to the ports so that they will not cause extra trauma to the patient.”
He has been fine-tuning the microlens technology for more than a decade and sought to transform his technology from the realm of sci-fi into clinically relevant applications. And for the past several years, Jiang has collaborated with laparoscopic surgeons at UW–Madison on ways to do just that.
“This whole project was generated and driven by both sides — from the pursuit to address engineering challenges to the pursuit to solve clinical and medical problems,” he says. “The advantage of our approach is that we gave the clinical requirements and disadvantages a lot of thought so that we could come up with a comprehensive solution to address all of the problems.”
“Rather than address incremental improvements, we came up with a paradigm shift to address all of the problems surgeons experience.”
Hongui Jiang
Jiang received a four-year, $1.6 million grant from the National Institutes of Health to fund the effort. In addition to Jiang and Heise, the UW–Madison research team includes Jacob Greenberg, an assistant professor of surgery; and Yu Hen Hu, a professor of electrical and computer engineering.
While the researchers have made significant strides, they will continue to refine the lens and camera technology. They also will focus on developing algorithms for processing the images from multiple cameras and stitching them seamlessly into a single, 3-D view, as well as developing prototypes for laparoscopic simulators that will allow them to gauge how surgeons use the system.
Heise says that if successful, the technology could expand to any number of minimally invasive surgery fields. “It’s a different way to approach this,” he says. “It’s out there a bit, and it’s something that will take refining for us to be able to use it clinically. But with Hongrui’s technology, it’s a possibility. I think it could really make a difference for us.”
Tags: engineering, health & medicine, research




