UW–Madison researchers reveal how key protein might help influenza A infect its hosts
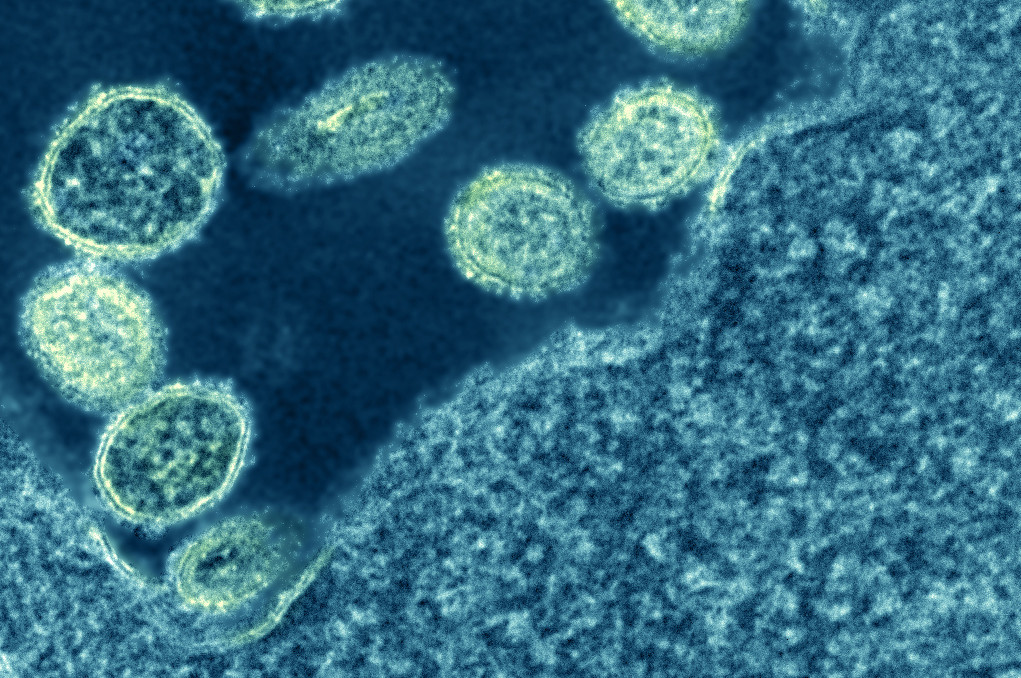
Through the magnification of an electron micrograph, particles of the 1918 pandemic’s influenza A virus crowd along the edge of a much larger host cell. National Institute of Allergy and Infectious Diseases
Influenza A is one of two influenza viruses that fuel costly annual flu seasons and is a near constant threat to humans and many other animals. It’s also responsible for occasional pandemics that, like the one in 1918, leave millions dead and wreak havoc on health systems and wider society.
Influenza A was first identified as a health threat nearly a century ago, but only in the last decade have scientists identified one of the virus’s key proteins for infiltrating host cells and short-circuiting their defenses. Now, a team of researchers at the University of Wisconsin–Madison have taken a major step toward understanding how that protein works, with a new finding that runs counter to previous conventional wisdom: They’ve found that viruses like influenza A take over host cells in a way that more closely resembles a tactical strike than brute force.
The protein in question is known as PA-X. It disrupts host cells by degrading their RNA — the genetic material cells need to make proteins for all sorts of purposes, including mounting a defense against invading viruses. PA-X makes thousands of cuts in the RNA of host cells, cleaving the cells’ genetic handbook into an indecipherable mess.
But viruses need to deploy this protein while also ensuring their own RNA remains functional. Scientists have been trying to understand how the influenza A virus takes over host cells while minimizing damage to itself. These competing priorities raise a fundamental quandary that gets to the heart of how influenza A has been able to remain such a persistent threat over the eons.

Marta Gaglia
“And that’s how the virus is able to mount a surgical strike for the host without messing up its own replication,” says Marta Gaglia, an associate professor of medical microbiology and immunology, describing the process by which the virus hijacks host cells to make copies of itself. Gaglia, who led the study, joined the faculty at UW–Madison’s Institute for Molecular Virology in 2022.
Using a form of genetic analysis known as high-throughput sequencing and some advanced statistical modeling, Gaglia and her colleagues believe they have cracked at least part of the secret that allows PA-X to degrade host cell RNA without doing too much collateral damage.
“It turns out that PA-X has a strong preference for a very specific sequence of RNA,” says Gaglia.
Crucially, Gaglia and her colleagues found that the RNA sequence that PA-X tends to target is very common in the genetic material of humans and other animals infected by influenza A viruses but rarely occurs in the virus’s own RNA. And while the protein’s aim isn’t perfect — it sometimes cuts through non-target RNA sequences — it seems to be good enough to do its job of disrupting the function of host cells. The findings are detailed in a new paper published June 22 in the journal Nature Microbiology.
In addition to identifying the specific RNA sequences that PA-X targets, the study suggests that the influenza A virus has a mechanism for differentiating between RNA sequences in the genetic material of its hosts and itself. This phenomenon, known as self/non-self recognition, is a well-documented part of hosts’ immune response to pathogens, but it hasn’t before been recognized in viruses.
“It’s interesting to see the virus also has found a way to do that, flipping the script,” says Gaglia.
Much about the precise function of PA-X remains unknown. Gaglia and her colleagues are looking into whether their current methods adequately capture the position and number of sites in the RNA sequences where PA-X makes its cuts. That work involves fine-tuning the group’s statistical models, which are the result of a collaboration with Gaglia’s husband, Christopher Rycroft, who is a UW–Madison math professor.
“We’ve collected some more datasets that we hope to use to refine the methods so we can make this a really robust program that other people can use to analyze their data as well,” Gaglia says.
Another open question about PA-X involves its role in the severity of an influenza infection. Previous studies have shown that influenza A strains with a less active PA-X protein are associated with more severe symptoms. But researchers have so far not been able to identify specific genetic hallmarks of a PA-X protein that indicate how active it might be.
“An ideal world that we would like to get to is: If you give me a sequence, I could take a look and say, ‘This is a really active version,’ or, ‘This is a less active version,'” says Gaglia. “And in simplistic terms, that could indicate whether it could be a more dangerous strain.”
Tags: influenza, microbiology, research, virology




