Faster, safer method zaps tumors with great success

Kevin McSweeney, a UW–Madison professor of soil science, leads a class field trip to the Arlington Agricultural Research Station in May. After undergoing a successful tumor ablation procedure at UW Hospital, McSweeney was back in the classroom within a couple of days.
When Kevin McSweeney was referred to UW Health last year for a tumor in his liver, he had already gone through six rounds of chemotherapy and 13 surgeries over 10 years to treat his metastasized cancer.
Rather than put him through another operation and round of radiation and chemo, his physicians decided to utilize a technology developed by UW scientists: microwave tumor ablation.
Tumor ablation techniques provide minimally invasive cancer therapies that involve destroying tumors with microwaves, freezing temperatures and electric currents as alternatives to more traditional surgical methods.
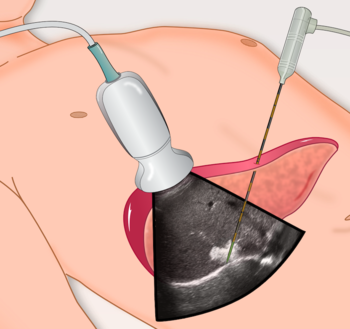
Image-guided therapies like this ultrasound-guided microwave ablation can be used to treat many cancers.
Illustration courtesy of Brace Group
“They had a multidisciplinary conference of physicians to analyze my case and decided I was a good candidate for ablation,” says McSweeney, a UW–Madison soil science professor. “I was very pleased because obviously conventional surgeries and chemotherapy are quite a drain on an individual.”
Rather than undergoing surgery to remove the liver tumor that would have left him recovering for several months, McSweeney says the ablation treatment allowed him to get back to his daily life quickly.
“From a patient’s perspective, this procedure is really wonderful because it’s very precise and the aftermath impacts are negligible,” McSweeney explains. “I didn’t have any discomfort, I was up the next day feeling fine and I was back in the classroom the day after.”
The procedure is virtually painless and takes less time than a typical surgery to remove a similar tumor. After the tumor has been located using an ultrasound, the physician inserts a probe (or up to three, depending on tumor size) into the tumor and directs the microwave energy to destroy the diseased tissue.
UW Health Chief of Abdominal Radiology Louis Hinshaw places microwave probes in a liver tumor using ultrasound guidance.
Photo courtesy of Fred Lee
Once the ablation is complete — typically under ten minutes — the physician removes the probe(s) and the patient is kept under supervision for the next day. From start to finish, the procedure lasts from one to two hours.
UW School of Medicine and Public Health radiologist Robert Turrel and Professor of Imaging Science Fred Lee founded the tumor ablation lab in 1995 after finding that most of the available ablation technology was severely underpowered and ineffective. Lee worked with Daniel van der Weide, a professor of electrical, computer and biomedical engineering; Chris Brace, one of van der Weide’s students and now an Associate Professor of Radiology and Biomedical Engineering; and Paul Laeseke, a graduate student and now a radiology resident at Stanford University, to build a better, more effective ablation tool.
“We really had to think outside of the medical space to get the equipment together in the first place,” says Brace.
Lee explains that because they were developing this technology from the ground up, they began with the most basic — and somewhat unorthodox — equipment: a microwave, WWII-era wave guides and hand-made antennas.

Chris Brace

Fred Lee
“This was totally bootstrapped from the ground up with nothing. Nothing preexisting in the field was available at the university, so we had to make it out of used and surplus equipment on our own time.”
After several years of developing and testing the microwave ablation device, Lee, van der Weide, Laeseke and Brace licensed the technology through the Wisconsin Alumni Research Foundation (WARF) in order to begin offering the treatment to patients. This license also allowed them to found NeuWave Medical, a Madison company that has expanded the reach of microwave ablation treatment all across the U.S., and soon to open in Canada and Europe by manufacturing the ablation device and marketing it to hospitals and clinics.
Brace says that although the UW was not the first place to use microwaves to destroy tumors, their approach took the idea from the initial research phase all the way to clinical applications.
“I think part of what makes us unique is that we are starting from the clinical problem and trying to engineer the solution directly,” Brace explains. “Many labs are focused on one tiny little thing, but we’re working on all different aspects of this discipline.”
“I didn’t have any discomfort, I was up the next day feeling fine and I was back in the classroom the day after.”
Kevin McSweeney
Patients from throughout the U.S. have come to UW Hospital seeking the expertise of radiologists trained in ablation therapy, and Lee says that he gets daily requests for treatment advice from physicians in other institutions.
“People come for this treatment from all over,” explains Lee. “There are places that do ablations well, but we specialize in it.”
In addition to it being an effective treatment, Lee says microwave tumor ablation is a less expensive option (although it is not covered by all insurance plans) when compared to traditional surgery, as well as safer: the rate of complications is typically under two percent, and most of the common complications are minor. At UW Hospital, radiologists have treated more than 300 patients with microwave ablation with a success rate of 95 percent in a single session.
McSweeney says that after receiving the ablative treatment, he has emphasized his positive experience to others. Since his last treatment in February, he has gone back for follow-up body scans, but no new tumors have developed.
“I think where it’s appropriate for someone undergoing cancer treatment, it’s a really great alternative to the other options,” says McSweeney. “Now that I know about it … I tell everybody I know, just so they know if this happens to them or someone who is close to them that they should explore the option.”
Tags: cancer, health & medicine, health care, research




