Veterinarians, physicians to jointly explore links between animal and human health
A physician, a veterinarian and a PhD researcher walk into a conference. At the event’s conclusion, the medical doctor says: “I had no idea there were veterinary cardiologists like there are human cardiologists.”
This interaction occurred at a translational health summit coordinated by the University of Wisconsin–Madison School of Veterinary Medicine in 2018 on the topic of inherited cardiomyopathies — diseases of the heart muscle — in people, cats and dogs. Now, the SVM has been awarded a five-year, $3 million grant from the National Institutes of Health to further bolster efforts to bring physicians and veterinarians together in support of human and animal health.
“Our goal is to leverage the skills of veterinary specialists and bring them into research teams, helping physicians and PhD researchers see that many of the diseases they study also occur in animals, and what veterinarians know about these diseases in animals can help advance treatment in people,” says Lauren Trepanier, professor and assistant dean for clinical and translational research in the SVM.
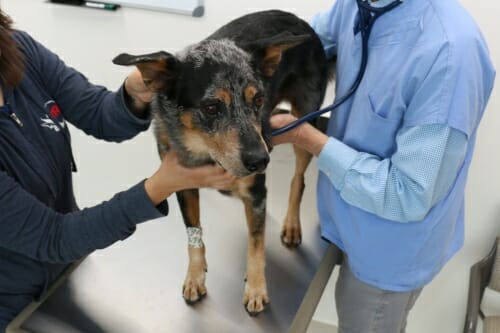
Senna, a 9-year-old Catahoula leopard dog, receives an exam at UW Veterinary Care as part of his treatment for cancer. The School of Veterinary Medicine has been awarded a grant to bring physicians and veterinarians together to advance knowledge of shared diseases across different species, such as cancer, osteoarthritis and epilepsy. Photo: Meghan Lepisto, UW–Madison
The grant will also help support the development of graduate veterinarians into skilled clinician-scientists and address gaps in knowledge of human and animal diseases.
Trepanier is principal investigator on the Translational Research Workforce Training grant, in coordination with Professor Christine Sorkness at the UW–Madison School of Pharmacy and partners in the Clinical and Translational Science Award One Health Alliance: Robert Rebhun at the University of California, Davis; Amara Estrada at the University of Florida; and Eva Furrow at the University of Minnesota.
The program aims to address several current shortfalls that have led to missed opportunities for veterinary clinicians and the field of translational medicine, Trepanier says. These include an inadequate number of research fellowships for veterinarians after residency training, a shortage of clinician-scientist role models and research mentors, and a lack of communication between veterinary and physician scientists regarding shared diseases across different species.
Because of their familiarity with the comparative aspects of disease, veterinarians are uniquely positioned to contribute expertise to translational research teams, Trepanier says.
“Veterinarians often understand similarities and differences between animal and human diseases because we go to the human medical literature all the time on the clinic floor. If we’re treating a disease in an animal and there’s no veterinary study, we look at a human study,” she says. “What we want physicians to do is look to veterinary medicine and see that there may be a disease that’s just like the disease in humans.”

Lauren Trepanier
The translational research training program will offer two-year funded fellowships for targeted research training for those just out of residency (advanced training in a variety of clinical specialties), without the commitment of pursuing an additional postgraduate degree. Participants can choose from a menu of fellowship opportunities, to begin in fall 2020, at 15 veterinary medical schools within the COHA network. Each fellowship mentor team will include a mix of MD, DVM, PhD and other specialists, and focus on diseases common to both veterinary and human patients.
For early-career veterinary faculty, a three-day COHA Translational Research Immersion Program — to be hosted for the first time in September 2019 in Madison and then biennially — will cover study development, grant writing, research implementation and more. Trainees will also receive mentoring for any planned grant proposals in the year following the immersion program.
This is intended to help equip veterinarians with more confidence as researchers, Trepanier explains. Many are hired into faculty positions with little research experience due to the high demand for certain clinical specialties in veterinary teaching hospitals.
“New faculty are expected to perform research and mentor residents, when maybe they came straight out of a residency themselves,” she says. “They have every ability to become an excellent researcher; they just need the skill set to feel as satisfied with their research life as they do with their clinical life.”
Finally, a series of COHA translational summits across the country will convene established veterinary and human medical researchers who are studying the same diseases. Planned topics range from skin allergies to cancer pain, osteoarthritis and epilepsy.
If we’re treating a disease in an animal and there’s no veterinary study, we look at a human study,” Trepanier says. “What we want physicians to do is look to veterinary medicine and see that there may be a disease that’s just like the disease in humans.”
“We’re bringing together clinicians and scientists from different walks of life to collaborate around shared disease interests and advance understanding of these conditions,” Trepanier says. “The idea is to see what each group can bring to the table to solve this problem and get veterinary researchers into larger teams.”
Two pilot summits funded by COHA grants to the SVM, including the 2018 workshop on cardiomyopathies, yielded positive feedback and new cross-professional collaborations, says Trepanier. “People said things like, ‘This is genius,’ ‘I’ve never been to anything like this before,’ and ‘This is a real eye-opener.’”
For Trepanier, who has mentored residents and new faculty for more than 20 years at the SVM, it’s gratifying to see support grow for training the next generation of veterinary clinician-scientists.
“The goal isn’t to have them lose their veterinary identity, but rather to keep that identity and bring it to the table in a new way — to help people see that they don’t have to give up being a clinician to do research and there’s satisfaction in treating patients individually, but also moving the field forward in a bigger way,” she says.
Tags: grants, health, veterinary medicine




