UW-Madison spinoff releases new module to help women, doctors decide on mammogram
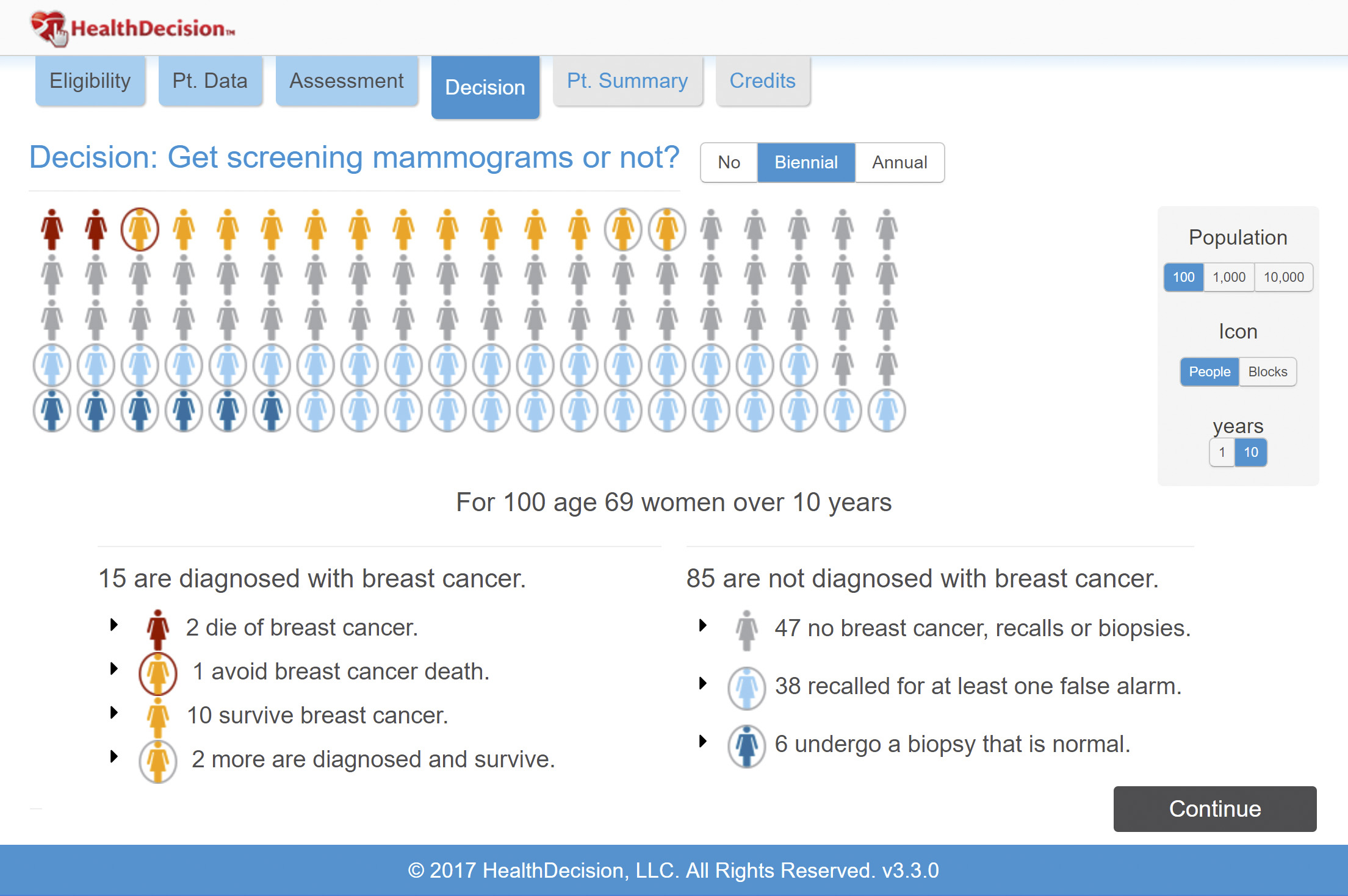
A screenshot from Health Decision software depicts the risk associated with getting a biennial mammogram screening for a 69-year-old woman with a familial history of breast cancer,. Patients and doctors find that these visuals help patients understand the risks and benefits of procedures.
HealthDecision, LLC, a 7-year old startup with deep roots at the University of Wisconsin–Madison, has just released the fourth module in a series intended to help doctors and patients share decisions.
The new breast cancer screening module, intended to help both parties assess whether a mammogram is appropriate, joins others aimed at specific questions concerning lung cancer, heart rhythms and cholesterol.
Although the software modules are designed for in-office use by doctors and patients, they are also available to the public at https://www.healthdecision.org/.

Jon Keevil
HealthDecision builds on evidence from the medical literature and tailors its results to the specific patient. The program window that opens within the patient’s electronic health record already contains patient data. The doctor can add missing data, such as a family history of cancer. Successive screens show how the effects of various choices (such as choosing or declining an annual mammogram) affect the probability of illness or death.
Tailoring risk factors to the patient can lead to surprises, says HealthDecision founder Jon Keevil, a cardiologist who practiced until recently at UW Health. “Many patients might assume that more frequent screening would automatically translate into a better health outcome, but we do the math and our graphic presentation helps them think through the situation.”
The approach could bring clarity to women trying to make sense of shifting recommendations on breast cancer screening. For many women, annual breast cancer screening will make some reduction in the projected 10-year death rate. But the program’s results will also illuminate the potential downside of regular screening: hundreds of “false positive” results that lead to worry and unnecessary biopsies.
“The advice for women aged 40 to 49 regarding screening mammograms is controversial and varied,” says Sarina Schrager, a physician and professor of family medicine and community health at UW–Madison who consulted on the breast cancer module.
A graphic display of the results of the program’s calculations “starts a conversation between the physician and patient, with the focus on what is important to the patient,” says Schrager, who practices in Madison. “It puts a different spin on the same information and facilitates shared decision-making within the relationship between the physician and the patient.”
“There is some data showing that patient satisfaction scores are higher if they use these tools,” Schrager says. “I find that patients love information, and they like to know ahead of time the potential for a particular test. I have not heard any negative feedback.”
Company founder Keevil majored in computer science and engineering as an undergraduate at Brown University. Deciding that he “wanted to do something more human-based,” he trained as a cardiologist and in 2000, joined the cardiology faculty at the School of Medicine and Public Health.
By then, the statistics-heavy field of “evidence-based medicine” was sweeping cardiology, like many other disciplines. And Keevil had already begun writing software to perform calculations that would apply medical evidence to individual patients.
“This was about helping myself and my colleagues do a better job,” Keevil says. “Then I waited 12 years for someone to build the cool tool that I envisioned, but nobody showed up, so I figured I’d have to build it myself.”
Beyond evidence-based medicine, the HealthDecision system supports another current concept in medicine: shared decision-making. The venerable “doctor knows best” attitude has been replaced, in many cases, with an emphasis on patients choosing from among the alternatives that the doctor has laid out. But with shared decision-making, the doctor brings medical expertise, and the patient brings intimate knowledge of what matters most.
Both Medicare and Medicaid have begun to require the use of shared decision-making in some situations.
HealthDecision software is designed as a plug-in module within a clinic’s electronic health record (EHR) system, such as Epic, Cerner and other health-record providers, Keevil says.
As a virtual company, HealthDecision’s 10 employees, including two who work full time, all telecommute. Funding has come from a range of sources, including Keevil’s personal investment, seed round financing, grants and UW Health. Expertise has come from specialists like Elizabeth Burnside, a professor of radiology in the UW School of Medicine and Public Health, Keevil says. HealthDecision is available within the EHR at UW Health and several other health-care systems.
Despite the profusion of health information software, HealthDecision occupies its own niche, Keevil says. “This is to be shared by the doctor and patient, it’s not a standalone for the patient. I felt the missing piece, for a lot of decisions, is help for the physician. These calculations can be hard for a physician to do during the typical clinic workflow. Our software crunches numbers in the background.”
Evidence will improve medicine only if it can be used, Keevil concludes. “Our tools are designed to be useful and effective for doctors, but their language is fairly simple, and the results are patient-friendly.”
Information and data are waiting to be used more fully, Keevil adds. “If we can help the doctor arrive at the best information, and present it in a way that the patient can see and understand, that is the most effective way to aid conversations on shared decision-making. I saw this as a way to have a larger impact on the field of medicine than I could taking care of patients individually.”
Subscribe to Wisconsin Ideas
Want more stories of the Wisconsin Idea in action? Sign-up for our monthly e-newsletter highlighting how Badgers are taking their education and research beyond the boundaries of the classroom to improve lives.